Practicing hand hygiene is a simple and effective way to prevent infections. Yet, according to the Centers for Disease Control and Prevention (CDC), health care providers on average clean their hands less than half of the times they should. Additionally, on any given day, about one in 31 hospital patients has at least one healthcare-associated infection (HAI).1
Limestone Medical Center, a 20-bed critical access facility in Groesbeck, Texas that employs 65 nurses, was concerned about its inability to obtain reliable data on hand hygiene compliance among health care workers throughout its system. The hospital’s original hygiene program relied on a direct observation monitoring system submitted via paper tools, and infection prevention staff felt the data was often invalid due to incomplete or inaccurate documentation.
“It was clear that in order to implement improvement processes or identify breakdowns in our hand hygiene program, we needed a comprehensive way to obtain insight,” according to Corey Tunnell, RN, CIC, Limestone’s infection preventionist. TMF Health Quality Institute, the Centers for Medicare & Medicaid’s Health Quality Improvement Contractor working with Limestone Medical Center, provided coaching and technical assistance throughout the selection and implementation of a new electronic hand hygiene electronic monitoring system.
Infrared Technology Promotes Hand Hygiene
With a grant from the Small Rural Hospital Improvement Program (SHIP) COVID-19 Testing and Mitigation Program, the facility purchased and implemented an electronic monitoring system in all patient care areas – encompassing exam rooms, inpatient rooms, radiology, lab draw rooms, therapy gyms, sleep study areas, and ancillary clinics – at the beginning of March 2022. The new monitoring system automatically documents each health care worker’s “upon entry” and “upon exit” hand hygiene moments, part of the “five moments of hand hygiene” recommended by the CDC and World Health Organization (WHO). A total of 63,987 moments were recorded in March, with a compliance rate of 96.01 percent.
The system employs beacons which use infrared technology to prompt the health care workers to perform hand hygiene. Each team member wears a badge with a hand that illuminates red (dirty hands), yellow (reminder to wash), and green (clean hands) which is visible to patients in real time – allowing the patient to be an active participant in their health care team.
Installation and Training
Installation and on-site training for the monitoring system took one week, with an average of 20 minutes of training per department. Staff training included a virtual component (video and online quiz) before one-on-one on-site training by the hospital infection preventionist and the vendor’s project success manager. After installation, feedback forms and routine rounding have allowed team members to discuss any concerns and reduce barriers to full integration of the system into their daily workflow.
1 “Hand Hygiene in Healthcare Settings,” Centers for Disease Control and Prevention, https://www.cdc.gov/handhygiene/index.html
Implementation and Early Lessons from the Data
Upon implementation, data revealed that Limestone had its lowest compliance rates during the “entry/before contacting a patient” moments. This information helped the facility target staff education efforts around this phase of hand hygiene. Additionally, staff discovered that the environmental services department experienced a significant rate of cross-contamination due to inappropriate personal protective equipment (PPE) use. Data from the new system enabled staff to investigate the situation, identify the user and barrier to compliance, and provide one-on-one education.
The purpose of data collection is not simply to meet regulatory requirements,” says Tunnell. “It is about what you can learn from the data and the opportunities you receive to improve your health care team's performance, ultimately increasing patient safety.”
Benefits of Electronic Monitoring System
The infection preventionist researched several products before selecting an electronic monitoring system. Part of the selection process included representatives of staff from each clinical department. The group participated in on-site demonstrations and were encouraged to offer feedback, which increased staff buy-in. Tunnell ultimately settled on a system because of its ease-of-use, cloud-based information storage, and inability to “cheat the system.” For example, an employee cannot falsify wearing their badge because the system identifies a target number of hand hygiene opportunities (HHO) based on job and department for each shift, so missed HHO targets or high rates of HHO exceptions are a red flag and generate a report for review and individual follow-up.
TMF Coaching Facilitates Implementation
TMF assisted Tunnell during this process by providing topic-specific data, one-on-one coaching on quality improvement best practices, and recommendations for effective presentations to stakeholders and decision-makers, specifically physician leadership and the hospital’s board of directors.
Although some of the clinical providers expressed initial hesitation, most staff welcomed the transition to an electronic monitoring system. TMF suggested an on-site demonstration with key frontline personnel or end users to be present which created early buy-in of the product. This also allowed each department to ask questions directly to the vendor and established involvement in implementation from the first step.
According to Tunnell, the facility is currently in the initial phase of monitoring system implementation, which consists of comparing the hours logged by the badge to the billing hours for each employee – an important measure of work flow integration and staff compliance with the program. In the next phase, Limestone will monitor user compliance within each facility department and recognize employees for meeting or exceeding compliance goals as positive reinforcement. The facility will also continue to monitor cross-contamination percentages in order to reduce potential HAIs related to improper practices.
Department Compliance
March – June 2022
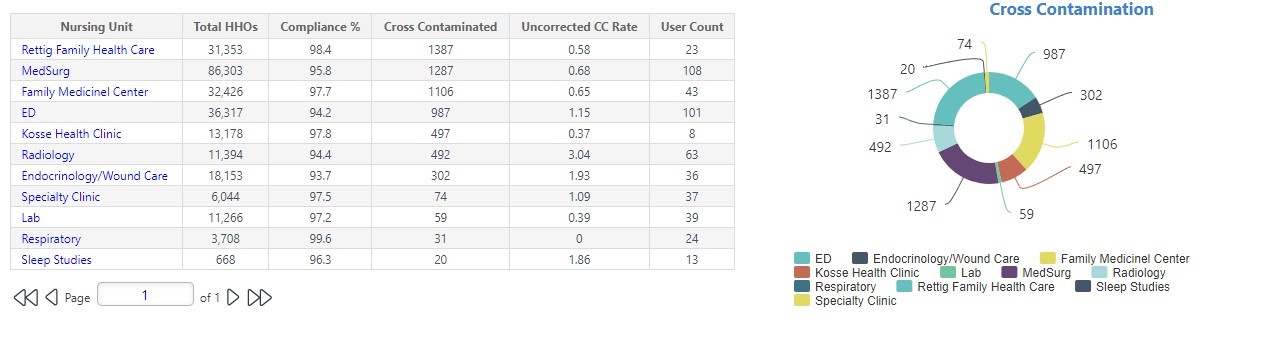
For more information on the hand hygiene electronic monitoring system used at Limestone Medical Center, contact:
Corey Tunnell, RN, CIC
Infection Preventionist, Limestone Medical Center
254-729-3281 Ext. 2281